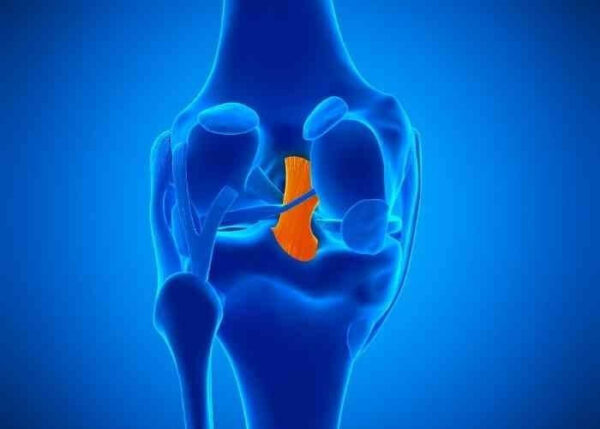
What and where is the PCL?
The PCL, also known as the Posterior Cruciate Ligament, is located on the back and middle of the knee. The PCL connects the femur (thigh bone) to the tibia (shin bone). It is the strongest ligament in the knee, giving it the advantage of being injured less often than the other ligaments. When the PCL is injured, it is usually due to a trauma, accident or severe fall. Sports like football, skiing, soccer and basketball, are often the main contributors to a posterior cruciate ligament injury. Dr. Armando Vidal, orthopedic knee specialist serving patients in Vail, Aspen and the surrounding Denver, Colorado communities has extensive experience in treating patients with a PCL injury.
What are the symptoms of a PCL Injury?
A PCL injury usually occurs from a direct impact to the front of the tibia (shin bone) such as a fall on a flexed (bent) knee or a dashboard injury. We also see them from mountain bike injuries here in the mountains. In addition, PCL injuries can occur in the setting of severe trauma where other ligaments are often involved in the injury. It’s not unusual for patients to seek help from another type of knee injury and discover the PCL is also stretched or torn. Some common symptoms of a posterior cruciate ligament injury are:
- Bruising and impact to the front of the tibia
- Swelling of the knee (usually mild)
- Instability with certain activities
- Difficulty walking downstairs
- Problems or difficulty when twisting, pivoting or turning
- Problems when slowing down from a run or increased pace
How is a PCL Injury diagnosed?
Dr. Vidal will perform a detailed clinical exam, medical history and background, including events leading up to the injury. X-rays and an MRI scan will determine the extent of the injury as well as other injuries inside the knee joint. In cases where the PCL injury is isolated, without further knee injuries, it can often heal over time without surgery. It is vital for patients in Vail, Aspen and the surrounding Denver, Colorado communities to receive a correct evaluation and diagnosis. This particular ligament tear needs to heal in a stable position, rather than in an elongated and nonfunctional position. Dr. Armando Vidal understands the intricacies of PCL injuries and how to treat them properly – both surgically and non-surgically. Some of tests he may use to test the PCL injury and the instability of the knee the injury has caused are:
- Posterior Drawer test: A specific maneuver used to test stability. With the patient lying down, Dr. Vidal will bend the knee while applying slight pressure and rotation. Some rotation is normal, and he will compare the degree of shift with the healthy knee.
- Dial Test: Tests knee stability. Dr. Vidal turns the foot outward. Excessive rotation can indicate a PCL injury.
- Assessment for a Varus Thrust Gait: In short, Dr. Vidal looks for a crooked knee, or for the knee to bow outward during adduction. (Adduction is the movement made when walking forward in a straight line).
- Quadriceps Active Test: Done with the knee bent, the patient pushes their lower leg forward using their quadriceps muscle while Dr. Vidal pushes against the movement at the ankle. The knee should not move forward noticeably through the movement.
Imaging is also very useful in diagnosing these injuries. Similar to posterolateral corner injuries, imaging can be tricky in PCL injuries. In acute injuries, an MRI can be reliable in indicating that an injury occurred, but in and of itself does not tell you the severity of the injury or if it is competent. In chronic injuries or in the setting of revision surgery – an MRI is not an accurate measure of how competent the PCL really is. In fact, in the chronic setting, the PCL can look totally normal on MRI. In these cases, a radiographic stress test will be performed. This essentially means that we will stress your knee (and your normal knee as a comparison) similar to what was done on physical examination and obtain an X-ray while performing the stress. Any asymmetry will be measured to determine functional integrity of the PCL. This is a key test and is the only objective measure of PCL integrity.
Are there different classifications for an injured PCL?
PCL injuries are classified using a grade system:
- Grade 1 injury: Sprained Ligament – small or partial tear, causes minimal instability in the knee tear.
- Grade 2 injury: Sprained Ligament – Tear of the ligament that is not quite a complete tear.
- Grade 3 injury: Complete tear of the ligament – the ligament does not function and other ligaments are most likely injured.
Grade 3 PCL injuries often require surgery due to the association with other ligament injuries and the low likelihood of healing. Grades 1 and 2 PCL injuries are almost universally managed non-operatively.
How is a PCL injury treated?
Non-Surgical Treatments:
Most PCL tears that are Grades 1 and 2 and do not have other ligament or soft-tissue damage can be treated non-surgically. Treatment can include:
- Brace to keep the tibia in a good position while the ligament heals. This minimizes any residual laxity or looseness once it heals
- RICE – Rest, Ice, Compression, Elevation
- Crutches are recommended to keep weight off of the injured knee in the first couple of weeks.
- Physical Therapy to improve range of motion and strength in the surrounding muscles and minimize load across the injured ligament.
Surgical Treatments:
Surgical treatment for a PCL injury needs to be done by a surgeon who has extensive experience in PCL reconstruction and repair. PCL injury infrequently occurs in isolation and Dr. Vidal carefully assesses the patient to determine any concurrent injury. Posterolateral corner, posteromedial injury, or the involvement of other ligaments can be common co-occurrences and needs to be addressed during the surgery.
Typically, PCL reconstruction requires an allograft (graft from cadaver) to reconstruct the PCL given its size and length. Similar to an ACL, tunnels are drilled in the tibia and the femur at the anatomic attachment sites of the PCL and the graft is passed and fixated under tension.
How long is the recovery after surgery for a posterior cruciate ligament reconstruction?
Recovery after PCL injury surgery will take time and patience, but most patients do well and are able to return to their regular activities. It is important to follow Dr. Vidal’s post-surgical protocol to achieve the maximum benefit and proper healing. In general, patients can expect the following:
- A bendable brace, known as a jack brace will be placed on the knee following surgery.
- Pain medications may be prescribed and should be taken exactly as directed.
- Vidal will have patients flexing their knee immediately after surgery, to maintain flexibility and range of motion.
- Crutches will be used for the first 6 weeks and weightbearing will begin slowly.
- Patients are weaned off of crutches slowly, with continued progress of walking without limping.
- After Dr. Vidal’s approval and proper healing, patients may begin using a stationary bike to build strength.
- Physical therapy will continue, with full recovery expected in about 6 months and a return to sporting activities in 12 months.
PCL Reconstruction Specialist
Have you experienced trauma to the knee resulting in pain, bruising, and a decreased range of motion? If so, you may be experiencing an injury to the PCL. Damage to the PCL must be assessed by an expert. Complex knee specialist, Doctor Armando Vidal provides diagnosis as well as treatment plans for patients in Vail, Aspen, and the surrounding Denver, Colorado communities who have experienced a recent knee injury. Contact Dr. Vidal’s team today!

Locations
180 S Frontage Rd W
Vail, CO 81657
226 Lusher Court
Ste 101
Frisco, CO 80443
322 Beard Creek Road
Edwards, CO 81632


